Remote patient monitoring tools are revolutionizing healthcare, empowering patients and providers alike. These tools offer a wide array of capabilities, from wearable devices to telehealth platforms, facilitating continuous health data collection and analysis. Understanding these tools, their benefits, and potential challenges is crucial for anyone involved in healthcare.
This guide delves into the intricacies of remote patient monitoring, exploring various aspects from implementation to future trends. We will examine the different types of RPM tools, their advantages, and the crucial role of data security and patient engagement.
Introduction to Remote Patient Monitoring Tools
Remote patient monitoring (RPM) tools are transforming healthcare by enabling continuous, real-time health data collection and analysis outside of traditional clinical settings. These tools empower patients and healthcare providers with valuable insights, facilitating proactive care and improved health outcomes. They offer a dynamic approach to patient care, fostering a more personalized and efficient healthcare experience.RPM tools encompass a wide range of technologies, from wearable sensors to telehealth platforms.
These systems collect and transmit health data, which is then analyzed to identify trends and provide insights into a patient’s condition. This allows for timely interventions and adjustments to treatment plans, leading to better patient management and improved health outcomes.
Types of Remote Patient Monitoring Tools
RPM tools utilize diverse technologies to collect and transmit health data. Wearable devices, such as smartwatches and fitness trackers, are increasingly popular for collecting physiological data like heart rate, activity levels, and sleep patterns. Telehealth platforms, which include video conferencing and secure messaging, provide a crucial communication channel for remote consultations, medication management, and support. Mobile applications offer a user-friendly interface for patients to access their health data, track progress, and communicate with their care team.
Key Features and Functionalities of RPM Tools
RPM tools are designed with specific features to facilitate efficient and effective patient care. Data collection and transmission are crucial elements, enabling continuous monitoring of vital signs, medication adherence, and activity levels. Real-time data analysis allows for proactive interventions and adjustments to treatment plans. Secure data storage and encryption protect patient privacy and confidentiality. Furthermore, the tools provide user-friendly interfaces for patients and healthcare providers, enabling seamless data access and communication.
Integration with existing electronic health records (EHRs) streamlines workflows and improves data consistency.
Examples of RPM Tool Use in Healthcare Settings, Remote patient monitoring tools
RPM tools are applied across various healthcare settings. In chronic disease management, RPM tools assist in monitoring patients with conditions like diabetes and hypertension, allowing for early detection of complications and adjustments to treatment plans. In post-operative care, RPM tools aid in monitoring patients’ recovery progress, enabling proactive interventions if complications arise. Remote monitoring of patients with mental health conditions helps track symptoms and provides support, ensuring timely interventions.
RPM tools also prove invaluable in preventative care by tracking health metrics and promoting healthy lifestyle choices.
Components of a Typical RPM System
A well-designed RPM system incorporates several key components to ensure efficient and reliable data collection and analysis.
| Component | Description |
|---|---|
| Patient Devices | These are the tools used by patients to collect and transmit data. Wearable sensors, smartphones, and tablets are common examples. |
| Data Transmission Network | This component ensures secure and reliable transmission of patient data to the monitoring center. Secure cloud-based platforms and dedicated networks are typically employed. |
| Monitoring Center | This is the hub for data collection, analysis, and communication. The center usually comprises trained personnel who analyze the data, identify trends, and communicate with patients and healthcare providers. |
| Data Analysis Software | This software analyzes the collected data, identifies trends, and alerts healthcare providers to potential issues. Machine learning algorithms can be incorporated for more advanced analysis. |
| Reporting and Communication System | This component enables the sharing of data insights with healthcare providers and patients. Automated reports and secure messaging platforms facilitate communication. |
Benefits of Utilizing RPM Tools
Remote patient monitoring (RPM) tools are revolutionizing healthcare by enabling continuous patient health tracking and proactive interventions. These systems empower patients with greater control over their health while providing healthcare providers with valuable insights to improve care. The benefits extend to healthcare systems as well, leading to cost savings and improved efficiency.RPM tools offer a significant advancement in patient care, allowing for early detection of potential health issues and timely interventions.
By providing real-time data, RPM empowers patients and healthcare providers to work collaboratively in managing chronic conditions and promoting overall well-being.
Benefits for Patients
RPM tools empower patients by providing them with a greater sense of control and agency in managing their health. They gain access to real-time health data, allowing them to track progress, adjust their lifestyle choices, and communicate effectively with their healthcare providers. This proactive approach to health management can lead to better self-management skills and a more positive patient experience.
- Improved Self-Management: Patients gain access to their health data, enabling them to actively participate in their care. This empowers them to make informed decisions and adjust their lifestyle choices, leading to better management of chronic conditions.
- Enhanced Communication: RPM facilitates seamless communication between patients and healthcare providers, fostering a collaborative relationship. This improved communication leads to faster responses to health changes and timely interventions.
- Increased Convenience and Accessibility: Patients can access their health data from anywhere, anytime, via mobile devices. This increased accessibility enhances convenience and encourages consistent engagement in their care.
- Proactive Health Monitoring: RPM tools allow patients to track vital signs and other health metrics regularly, promoting early detection of potential issues. This proactive monitoring can prevent complications and lead to better health outcomes.
Benefits for Healthcare Providers
RPM tools provide healthcare providers with valuable data insights to improve patient care and reduce hospital readmissions. The data collected allows for proactive interventions, enabling timely adjustments to treatment plans and reducing unnecessary hospitalizations.
- Proactive Intervention: RPM tools enable providers to identify potential health issues early, facilitating timely interventions and preventing complications. For example, if a patient’s blood pressure readings consistently rise, a provider can intervene proactively, potentially preventing a hypertensive crisis.
- Enhanced Treatment Effectiveness: RPM data can help providers fine-tune treatment plans based on real-time patient responses. This data-driven approach ensures that treatments are effective and tailored to individual needs, maximizing positive outcomes.
- Improved Decision-Making: Access to comprehensive patient data allows providers to make more informed decisions about patient care. This data-driven approach supports personalized care plans and optimized treatment strategies.
- Reduced Hospital Readmissions: Early detection of potential health issues through RPM enables timely interventions, reducing the risk of hospital readmissions. This leads to cost savings for healthcare systems.
Benefits for Healthcare Systems
RPM tools can significantly impact healthcare systems by optimizing resource allocation, reducing costs, and improving overall efficiency.
- Cost Savings: RPM can reduce hospital readmissions, decrease emergency room visits, and optimize resource allocation. These factors lead to substantial cost savings for healthcare systems, making RPM a valuable investment.
- Improved Efficiency: RPM streamlines workflows, enabling healthcare providers to focus on high-value tasks. The automation of data collection and analysis frees up staff time for direct patient care.
- Enhanced Patient Outcomes: By facilitating proactive interventions and personalized care, RPM leads to better patient outcomes, reducing long-term healthcare costs.
- Increased Access to Care: RPM tools can expand access to care, particularly in underserved areas, by enabling remote monitoring and management of patients.
Examples of Improved Patient Outcomes Using RPM Tools
Studies have shown that RPM tools can significantly improve patient outcomes for various chronic conditions, such as diabetes and heart failure. For example, one study demonstrated a reduction in hospital readmissions for heart failure patients monitored using RPM tools.
Comparison of Benefits of Different RPM Tools
| RPM Tool | Patient Benefits | Provider Benefits | System Benefits |
|---|---|---|---|
| RPM Tool A | Improved self-management, enhanced communication | Proactive interventions, improved decision-making | Cost savings, improved efficiency |
| RPM Tool B | Increased accessibility, proactive monitoring | Enhanced treatment effectiveness, reduced hospital readmissions | Expanded access to care, optimized resource allocation |
| RPM Tool C | Personalized care plans, better support | Data-driven care, improved patient engagement | Reduced costs, improved outcomes |
Challenges and Limitations of RPM Tools

Remote patient monitoring (RPM) tools offer significant potential for improving patient care, but their implementation is not without challenges. These limitations can impede widespread adoption and optimal outcomes. Understanding these hurdles is crucial for developing effective strategies to overcome them and maximize the benefits of RPM.
Technical Challenges in Implementing RPM Tools
Implementing RPM tools often presents technical obstacles. Integration with existing electronic health record (EHR) systems can be complex and time-consuming, requiring significant upfront investment in both resources and expertise. Interoperability issues between different RPM platforms and devices can also create difficulties in data exchange and analysis. Ensuring the reliability and security of data transmission channels is paramount to maintain the integrity and confidentiality of patient information.
Moreover, the need for robust, reliable, and accessible communication infrastructure in remote areas can be a significant challenge. In some cases, a lack of technical support for both healthcare providers and patients can create a barrier to effective RPM implementation.
Security and Privacy Concerns Associated with RPM
Patient data collected through RPM tools is highly sensitive and vulnerable to various security risks. Unauthorized access, data breaches, and misuse of personal information are potential threats. Robust security measures, including encryption, access controls, and regular security audits, are essential to safeguard patient data. Maintaining patient privacy in accordance with regulations like HIPAA is critical and must be addressed during the design and implementation phases.
Ensuring compliance with data protection regulations is crucial to maintain public trust and avoid legal repercussions. A secure and private environment for RPM data is essential for the safety and efficacy of the system.
Challenges Related to Patient Engagement and Adherence
Patient engagement and adherence to RPM protocols are vital for the success of any RPM program. Lack of patient motivation, understanding, or trust in the technology can hinder their participation. Factors like convenience, ease of use, and the perceived value of the program directly impact patient engagement. Furthermore, the technology must be accessible and usable by patients with varying technical literacy levels.
Effective communication strategies, clear instructions, and ongoing support are necessary to foster patient engagement and adherence. Offering incentives and recognition can also be valuable motivators.
Challenges of Data Management and Analysis in RPM
The volume and variety of data generated by RPM tools can pose significant challenges for data management and analysis. Developing robust data management systems capable of handling large datasets and ensuring data quality is crucial. Standardization of data formats and protocols is essential for accurate analysis and reporting. Utilizing advanced analytics and machine learning algorithms to extract meaningful insights from the data can provide valuable information for personalized care and decision-making.
Data security and privacy must be maintained throughout the entire data lifecycle, from collection to analysis and reporting. This involves establishing clear policies and procedures for data handling, storage, and access.
Potential Security Risks and Mitigation Strategies
| Security Risk | Mitigation Strategy |
|---|---|
| Unauthorized Access | Strong passwords, multi-factor authentication, access controls, regular security audits |
| Data Breaches | Robust encryption, secure data storage, incident response plan, regular vulnerability assessments |
| Malware Attacks | Antivirus software, regular software updates, firewalls, intrusion detection systems |
| Phishing Attacks | Employee training on phishing awareness, secure email practices, strong password policies |
| Data Loss | Regular backups, data redundancy, disaster recovery plan |
Patient Engagement and Adoption
Patient engagement is critical for the successful implementation of Remote Patient Monitoring (RPM) tools. High engagement translates to better adherence to treatment plans, improved health outcomes, and reduced healthcare costs. Understanding the factors that influence patient adoption and developing strategies to foster positive experiences are essential for maximizing the value of RPM.
Strategies to Enhance Patient Engagement
Patient engagement with RPM tools can be significantly improved by focusing on clear communication, user-friendliness, and building trust. These strategies, when implemented effectively, lead to higher rates of tool adoption and sustained use.
- Intuitive User Interface Design: A user-friendly interface is paramount. RPM platforms should be easily navigable, with clear instructions and prompts. Visual aids, such as graphs and charts, can effectively display patient data and progress. Avoid overly technical jargon, ensuring the language used is easily understandable for patients with varying levels of digital literacy.
- Personalized Communication: Tailoring communication to individual patient needs is crucial. This can include personalized messages, reminders, and educational materials. Proactive communication, such as regular check-ins and updates, helps patients feel supported and informed. This approach fosters a sense of partnership between the patient and the healthcare provider.
- Providing Comprehensive Support: Patients should have access to ongoing support throughout their engagement with the RPM system. This could include readily available FAQs, online tutorials, or dedicated support staff available via phone or email. Addressing concerns and providing clear guidance ensures that patients feel empowered to use the tool effectively.
- Incentivizing Participation: Offering incentives, such as rewards or recognition, can motivate patients to use the RPM tools regularly. This can range from small rewards to significant discounts or opportunities for recognition within the patient community.
Examples of User-Friendly Interfaces
Effective RPM interfaces are designed to be both informative and engaging. They should visually represent data in an easily digestible format, enabling patients to understand their health status quickly. A well-designed interface fosters a positive experience, encouraging continued use.
- Dashboard-Style Displays: Clear dashboards that summarize key health metrics in a concise format can be very helpful. These dashboards could visually represent trends in blood pressure, weight, or other vital signs. The use of color-coded indicators can highlight deviations from normal ranges.
- Interactive Graphs and Charts: Visual representations of data, such as graphs and charts, allow patients to easily track their progress over time. Interactive elements, enabling patients to zoom in on specific data points or explore trends, further enhance understanding and engagement.
- Simplified Navigation: A simple and intuitive navigation structure is essential. Patients should be able to easily access the information they need without confusion or frustration. Clear labels and well-organized menus contribute to a seamless user experience.
Building Trust and Confidence
Trust and confidence in RPM tools are crucial for successful adoption. Transparency, clear communication, and demonstrated value contribute significantly to establishing this trust.
- Open Communication Channels: Open communication channels between patients and healthcare providers are essential for addressing concerns and questions. Patients should feel comfortable reaching out to their care team with questions or feedback.
- Transparency in Data Use: Transparency regarding how collected data is used is critical. Patients should understand that their data is being used to improve their care and not for any other purpose. Clear privacy policies and data security protocols should be readily available.
- Demonstrating Value and Outcomes: RPM tools should be presented as a valuable resource that improves health outcomes. Providing examples of how RPM has helped other patients or illustrating its impact on health metrics can help build confidence in the tool.
The Role of Education and Support
Education and support play a vital role in the adoption of RPM tools. Providing clear information and ongoing assistance helps patients feel comfortable and confident in using the tools.
- Comprehensive Training: Providing comprehensive training on how to use the RPM tool is essential. Training should include both hands-on practice and clear instructions, ideally offered in multiple formats (videos, written materials, and demonstrations). This ensures that patients are fully equipped to utilize the system.
- Regular Check-ins and Feedback: Regular check-ins with patients allow healthcare providers to address any questions or concerns they may have. Providing feedback on their progress and addressing any difficulties promptly is essential.
- Accessible Support Resources: Providing accessible support resources, such as FAQs and online tutorials, helps patients feel empowered to use the system independently.
Assessing Patient Satisfaction
Assessing patient satisfaction with RPM tools is critical for continuous improvement. Collecting feedback and evaluating satisfaction levels helps identify areas for enhancement and ensure that the tools meet patient needs.
- Surveys and Questionnaires: Regular surveys and questionnaires can gauge patient satisfaction levels regarding the user interface, functionality, and support services provided. These tools can help identify specific areas where improvements are needed.
- Focus Groups and Interviews: Focus groups and interviews with patients provide valuable insights into their experiences with the RPM tools. Direct feedback from patients can help uncover areas of improvement and identify specific issues.
- Monitoring Feedback Mechanisms: Utilizing existing feedback mechanisms, such as online forums or comment sections, can provide real-time insights into patient experiences with RPM tools. This allows for rapid identification and resolution of issues.
Integration with Existing Healthcare Systems
Integrating remote patient monitoring (RPM) tools into existing healthcare infrastructure is crucial for seamless data flow and improved patient care. This integration process must consider the unique needs of various healthcare settings, ensuring compatibility and interoperability with existing Electronic Health Records (EHR) and other systems. Successful integration streamlines workflows, reduces manual data entry, and enhances the overall efficiency of care delivery.
Process of Integration
The integration process typically involves several key steps, starting with careful planning and assessment of the existing IT infrastructure. This includes identifying the specific RPM tools and features that align with the organization’s needs and workflow. Data mapping is essential to define how RPM data will be linked to existing patient records. The integration should also consider security protocols and data privacy regulations to protect patient information.
Importance of Interoperability
Interoperability between RPM systems is critical for seamless data exchange and analysis. This ensures that data from different RPM platforms can be readily accessed and utilized by healthcare providers and support staff, regardless of the specific tool used. Lack of interoperability can lead to fragmented data, hindering comprehensive patient care and potentially causing delays in treatment decisions.
Examples of Successful Integrations
Several successful integrations have demonstrated the benefits of RPM tools within existing EMR systems. One example involves an integration where wearable devices automatically upload patient activity data directly into the EHR, enabling clinicians to track trends and adjust treatment plans accordingly. Another example highlights an integration of a remote blood pressure monitoring system that feeds data directly into the patient’s EMR, enabling prompt identification of potential issues and enabling proactive interventions.
Remote patient monitoring tools are becoming increasingly popular, but alongside the benefits come some crucial privacy considerations. These tools often collect sensitive health data, raising legitimate concerns about data security and how this data is handled, especially in the context of privacy concerns in modern tech. Ultimately, robust data protection measures are essential for the responsible implementation of remote patient monitoring tools.
Challenges in Integrating Diverse RPM Tools
Integrating diverse RPM tools can present significant challenges, including varying data formats and communication protocols. Different RPM systems may use incompatible data structures or communication methods, leading to difficulties in transferring data between platforms. Ensuring that these disparate systems can exchange information in a standardized manner is essential to overcome these challenges. Furthermore, maintaining data security and privacy across various systems is another crucial aspect to address.
Table: Steps in Integrating RPM Tools
| Step | Description |
|---|---|
| 1. Needs Assessment | Define the organization’s needs, identify suitable RPM tools, and assess existing IT infrastructure. |
| 2. Data Mapping | Establish the rules and standards for transferring data between RPM and existing systems. This includes defining which data points are crucial to capture and how they will be mapped to the existing EHR system. |
| 3. System Compatibility | Verify the compatibility of RPM tools with existing healthcare systems. This includes assessing the technical specifications, data formats, and communication protocols. |
| 4. Security & Privacy | Implement robust security measures to protect patient data during the integration process. This includes adhering to HIPAA regulations and other relevant privacy standards. |
| 5. Testing & Validation | Thoroughly test the integration process to ensure data accuracy, security, and reliability. This includes testing data transfers and functionality in a controlled environment. |
| 6. Deployment & Training | Deploy the integrated RPM system and provide training to staff on its use and maintenance. |
Data Security and Privacy in RPM
Remote patient monitoring (RPM) tools offer significant advantages for patient care, but safeguarding sensitive patient data is paramount. Robust security measures are crucial to build trust and maintain compliance with regulations. Data encryption, access controls, and rigorous privacy policies are essential components of a secure RPM system.Data privacy in RPM systems is a critical aspect that requires careful consideration.
The sensitive health information collected through these systems must be protected from unauthorized access, use, or disclosure. Implementing strong security protocols and adhering to relevant regulations is vital to maintaining patient trust and avoiding potential legal ramifications.
Importance of Data Encryption and Access Controls
Protecting patient data is paramount in RPM. Data encryption transforms readable data into an unreadable format, rendering it inaccessible to unauthorized individuals. Access controls restrict data access to only authorized personnel, ensuring that only those with a legitimate need to view patient information can do so. Implementing these measures is vital to preventing unauthorized access and data breaches.
Robust encryption algorithms and multi-factor authentication mechanisms are essential components of a secure RPM system.
Methods for Ensuring Patient Data Confidentiality
Several methods can ensure patient data confidentiality in RPM. Implementing strong access controls, including user authentication and authorization protocols, limits access to only authorized personnel. Employing data encryption throughout the data lifecycle, from collection to storage to transmission, is crucial. Regular security audits and penetration testing can identify vulnerabilities and address them proactively. Secure data storage solutions, including data backups and disaster recovery plans, are essential to protect against data loss or breaches.
Compliance with HIPAA and Other Relevant Regulations
Adherence to HIPAA (Health Insurance Portability and Accountability Act) and other relevant regulations is mandatory for RPM systems. HIPAA mandates specific safeguards for protecting electronic protected health information (ePHI). RPM systems must comply with these requirements to avoid penalties and maintain patient trust. This includes implementing security measures such as encryption, access controls, and audit trails. Organizations should also ensure that their data privacy policies align with applicable state and regional regulations.
Data Breach Prevention Strategies
Proactive measures are essential to prevent data breaches in RPM systems. Regular security awareness training for personnel involved in handling patient data can help prevent unintentional security breaches. Implementing strong passwords, multi-factor authentication, and regular software updates helps reduce the risk of exploitation. Incident response plans should be developed and regularly tested to ensure a swift and effective response to any security incidents.
Regular vulnerability assessments and penetration testing can identify and address potential weaknesses.
Comprehensive Overview of Data Privacy Policies for RPM
A comprehensive data privacy policy for RPM should clearly Artikel the organization’s commitment to protecting patient data. The policy should detail the types of data collected, how it is used, and who has access to it. It should specify the procedures for data security, access controls, and data retention. The policy should address data breaches, including reporting requirements and procedures.
The policy should be easily accessible to patients and clearly communicated to all staff involved in the RPM process. The policy should be regularly reviewed and updated to reflect evolving privacy regulations and best practices.
Data Analysis and Reporting
Remote patient monitoring (RPM) tools generate a wealth of data. Effective analysis of this data is crucial for deriving actionable insights, optimizing patient care, and ultimately improving health outcomes. Transforming raw data into meaningful reports and visualizations empowers healthcare providers to make informed decisions and enhance the overall efficiency of the patient care process.
Methods for Analyzing RPM Data
Various methods are employed for analyzing RPM data, each offering unique insights. These methods typically involve a combination of descriptive statistics, predictive modeling, and data visualization techniques. Common methods include:
- Descriptive Statistics: Summarizing key characteristics of the data, such as calculating averages, standard deviations, and frequencies, provides a baseline understanding of patient trends. For instance, average blood pressure readings, heart rate variability, and sleep patterns over time can be analyzed using descriptive statistics.
- Trend Analysis: Identifying patterns and changes in data over time is essential for monitoring patient progress. This can involve visualizing trends using line graphs or identifying anomalies in vital sign readings. For example, an upward trend in blood glucose levels over several weeks could signal a need for adjustment in treatment plans.
- Statistical Modeling: Statistical models can identify relationships between different variables and predict future outcomes. For instance, a regression model might predict the likelihood of a patient experiencing a hospitalization based on various RPM data points.
Examples of Actionable Insights
RPM data can reveal numerous actionable insights, directly impacting patient care. These insights can be used to prevent hospital readmissions, improve adherence to treatment plans, and personalize care strategies.
- Early Detection of Deterioration: Identifying unusual patterns in RPM data can alert healthcare providers to potential health issues early on, allowing for timely interventions. For example, a sudden drop in heart rate or a significant increase in blood pressure could indicate a developing complication.
- Improved Treatment Adherence: Analyzing patient engagement with the RPM system can provide insights into treatment adherence. Regular data transmission from patients can highlight areas where patients need support or education to enhance adherence to medication regimens or lifestyle changes.
- Personalized Treatment Strategies: Tailoring treatment plans based on individual patient data gathered from RPM devices allows for more personalized care. For example, adjusting insulin dosages based on real-time blood glucose readings or prescribing specific exercises based on heart rate responses can significantly improve treatment efficacy.
Generating Reports and Visualizations
Effective reporting and visualization are crucial for conveying insights derived from RPM data to healthcare professionals. Visual representations of data facilitate quicker comprehension and aid in identifying critical trends. Reports should be tailored to the specific needs of the users, whether it is for clinicians, administrators, or patients themselves.
- Data Visualization Tools: Utilizing interactive dashboards, charts, and graphs enables the easy visualization of trends, patterns, and outliers in RPM data. Tools like Tableau and Power BI are often used for this purpose.
- Customizable Reports: Reports can be customized to present data in a format that best suits the intended audience. For example, reports could focus on specific patient groups, highlight particular metrics, or summarize data across various time periods.
- Automated Reporting: Automated reporting systems streamline the process of generating regular reports and can be scheduled to provide timely updates. This allows healthcare providers to stay informed about the patients’ conditions without manual intervention.
The Role of AI and Machine Learning in RPM Data Analysis
Artificial intelligence (AI) and machine learning (ML) algorithms are increasingly used to analyze RPM data, enabling more accurate predictions and proactive interventions. These technologies can identify complex patterns and relationships in large datasets, which are often difficult for human analysts to recognize.
- Predictive Modeling: AI and ML algorithms can be trained to predict potential health issues or adverse events based on historical RPM data. This proactive approach allows healthcare providers to intervene before problems escalate.
- Personalized Recommendations: Algorithms can provide personalized recommendations for treatment adjustments or lifestyle modifications based on an individual’s RPM data and medical history. This can help improve patient outcomes and adherence to care plans.
- Anomaly Detection: AI and ML can identify unusual patterns or anomalies in RPM data that might indicate a developing health issue. This early detection can lead to prompt interventions and prevent potential complications.
Data Analysis Techniques for RPM
This table Artikels various data analysis techniques applicable to RPM data:
| Technique | Description | Example |
|---|---|---|
| Descriptive Statistics | Summarizes data characteristics (mean, median, standard deviation). | Average heart rate, blood pressure range. |
| Trend Analysis | Identifies patterns in data over time. | Monitoring blood glucose levels over weeks. |
| Statistical Modeling | Establishes relationships between variables. | Predicting risk of hospitalization based on vital signs. |
| Machine Learning (Classification) | Categorizes data into predefined groups. | Identifying patients at high risk for complications. |
| Machine Learning (Regression) | Predicts continuous outcomes. | Forecasting future blood pressure readings. |
Cost-Effectiveness of RPM Tools
Remote patient monitoring (RPM) tools offer a potential pathway to more cost-effective healthcare delivery. By enabling proactive health management and early intervention, RPM can reduce hospital readmissions, emergency room visits, and the need for expensive in-patient care. This, in turn, can translate to significant savings for healthcare systems and patients alike.
Comparing Costs of Implementing RPM Tools with Traditional Methods
Traditional methods of patient care often involve reactive interventions, meaning treatment is initiated only after a problem arises. This reactive approach can lead to increased costs due to delayed diagnosis, escalated treatment needs, and potential complications. RPM, in contrast, allows for proactive monitoring, potentially identifying and addressing issues before they become critical. This shift from reactive to proactive care is a key factor in the cost-effectiveness of RPM.
Detailed Analysis of Return on Investment (ROI) of RPM Tools
Determining the ROI of RPM tools requires careful consideration of various factors. These include the initial investment in hardware, software, and training, the ongoing operational costs (such as data management and personnel), and the potential savings from reduced healthcare utilization. A thorough analysis should quantify the expected reductions in hospitalizations, emergency room visits, and physician office visits. Real-world case studies can provide valuable insights into the financial impact of RPM programs.
Examples include projects where RPM was implemented to manage chronic conditions like diabetes or heart failure, demonstrating quantifiable reductions in healthcare costs.
Long-Term Cost Savings Associated with RPM
RPM tools offer significant long-term cost savings. By enabling continuous monitoring and early intervention, RPM can reduce the frequency and severity of acute exacerbations, leading to lower overall healthcare costs over time. This proactive approach can also improve patient outcomes, leading to improved quality of life and potentially reduced long-term care needs.
Case Studies of Successful Cost-Effective Implementations of RPM
Several healthcare systems have successfully implemented RPM programs and experienced demonstrable cost savings. One example might involve a program designed to manage chronic respiratory conditions, showing reductions in hospitalizations and emergency room visits. A successful program often includes clear goals, a well-defined target population, and appropriate data analysis to track outcomes and refine the program. Careful selection of appropriate RPM tools, tailored to the specific needs of the target population, is also critical for success.
Table Comparing Costs of Different RPM Solutions
| RPM Solution | Initial Setup Cost (USD) | Monthly Subscription Fee (USD) | Training Costs (USD) | Data Management Costs (USD) |
|---|---|---|---|---|
| Solution A | 10,000 | 500 | 2,000 | 100 |
| Solution B | 15,000 | 750 | 3,000 | 150 |
| Solution C | 20,000 | 1,000 | 4,000 | 200 |
Note: The costs in the table are illustrative and may vary based on specific features, functionalities, and implementation details. The table highlights the varying costs of different RPM solutions. Factors influencing cost include complexity, functionality, scalability, and ongoing maintenance.
Future Trends in Remote Patient Monitoring
Remote patient monitoring (RPM) is rapidly evolving, driven by technological advancements and the increasing need for accessible and personalized healthcare. This evolution promises to reshape the future of healthcare delivery, offering improved patient outcomes and cost-effectiveness. The integration of innovative technologies is transforming RPM, making it more comprehensive and efficient.
Emerging Technologies and Innovations
The field of remote patient monitoring is experiencing a surge in innovative technologies, fostering greater personalization and efficiency in healthcare delivery. These advancements are driven by the need for more proactive and preventative care models, enabling early intervention and improved patient outcomes. Key areas of innovation include the development of more sophisticated wearable sensors, improved data analysis techniques, and the integration of artificial intelligence (AI).
Wearable Sensors and IoT Devices in RPM
Wearable sensors and Internet of Things (IoT) devices are becoming increasingly sophisticated, enabling continuous monitoring of vital signs and activity levels. These devices are pivotal in capturing real-time patient data, facilitating timely interventions and promoting proactive healthcare management. For instance, smartwatches equipped with heart rate monitors, activity trackers, and blood oxygen sensors can provide comprehensive physiological data, enabling healthcare providers to monitor patients remotely and respond quickly to any anomalies.
This continuous data stream can be used to identify trends and patterns, enabling early detection of potential health issues and facilitating proactive interventions.
AI Utilization in RPM
Artificial intelligence (AI) is playing an increasingly significant role in RPM. AI algorithms can analyze vast amounts of patient data, identify patterns, and predict potential health issues. This predictive capability can help healthcare providers proactively intervene and improve patient outcomes. For example, AI-powered algorithms can analyze patient data from wearables and other sources to identify individuals at risk of developing chronic conditions like diabetes or heart disease.
This early identification allows for prompt interventions and preventive measures, ultimately improving patient well-being and reducing healthcare costs.
Predictive Modeling in RPM
Predictive modeling in RPM leverages historical patient data and machine learning algorithms to forecast future health risks and outcomes. By identifying patterns and trends in patient data, predictive models can anticipate potential health issues and enable proactive interventions. For instance, a model trained on patient data might predict the likelihood of a patient experiencing a heart attack based on factors like blood pressure, cholesterol levels, and exercise habits.
This predictive capability allows healthcare providers to intervene early, potentially preventing adverse events.
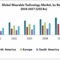
Future Growth of the RPM Market
The RPM market is projected to experience substantial growth in the coming years. The increasing prevalence of chronic diseases, coupled with the rising adoption of technology in healthcare, are key drivers of this growth. Factors such as the growing demand for personalized medicine, the cost-effectiveness of RPM, and the need for improved patient outcomes are expected to fuel market expansion.
Further, the decreasing costs of wearable sensors and the development of more sophisticated AI algorithms are contributing to this growth. Countries with aging populations and growing healthcare costs are likely to see significant growth in the RPM market.
Comparison of Different RPM Platforms
Remote patient monitoring (RPM) platforms are proliferating, offering diverse functionalities and capabilities. Choosing the right platform is crucial for effective implementation and optimal patient outcomes. This section delves into the comparative analysis of prominent RPM platforms, highlighting their key features, functionalities, strengths, and weaknesses. A comprehensive table summarizing these platforms is also provided.Various factors influence the selection of an RPM platform, including the specific needs of the healthcare provider and the patients they serve.
These platforms differ in their functionalities, pricing models, and user interfaces. This comparison aims to provide clarity in selecting the most suitable RPM platform.
Key Features and Functionalities
Different RPM platforms offer varying sets of features, catering to specific patient needs and healthcare provider requirements. Essential functionalities often include remote monitoring of vital signs, medication adherence tracking, and communication tools for remote consultations. Advanced platforms may include integration with electronic health records (EHRs), predictive analytics, and personalized treatment plans.
- Vital Signs Monitoring: Many platforms offer real-time monitoring of blood pressure, heart rate, weight, and other vital signs. This continuous data collection enables early detection of potential health issues and allows for proactive interventions.
- Medication Adherence: Automated reminders and tracking systems help patients remember to take their medications as prescribed. This feature is critical in managing chronic conditions and improving treatment outcomes.
- Remote Consultations: Video conferencing and messaging capabilities facilitate remote consultations between patients and healthcare providers. This improves access to care, especially for patients in remote areas.
- Data Integration: Integration with existing EHR systems ensures seamless data flow and reduces data duplication. This streamlines workflows and enhances data accuracy.
- Reporting and Analytics: Comprehensive reporting and data analysis tools provide insights into patient trends and outcomes. These insights are essential for optimizing care strategies and resource allocation.
Detailed Platform Specifications
This section Artikels the key features and functionalities of a few leading RPM platforms. Specific examples include detailed functionalities like the ability to track blood glucose levels, heart rhythm, and sleep patterns. Platforms may vary in their functionalities and pricing models.
- Platform A: This platform excels in vital signs monitoring and remote communication. It offers a user-friendly interface and robust integration capabilities. Data security is a key strength, with advanced encryption protocols in place. However, its reporting features might be limited compared to other platforms.
- Platform B: Platform B stands out for its comprehensive data analysis and predictive modeling capabilities. It provides valuable insights into patient trends, enabling proactive interventions. However, its integration with existing EHR systems may be less seamless than Platform A.
- Platform C: Platform C emphasizes patient engagement through gamification and personalized feedback. This approach can significantly improve patient motivation and adherence to treatment plans. However, it may lack the advanced analytical capabilities of Platform B.
Strengths and Weaknesses
Each platform possesses unique strengths and weaknesses. A platform’s strengths may include robust data security, seamless integration with existing healthcare systems, or a user-friendly interface. Conversely, weaknesses might include limited data analysis tools, high pricing, or a complex user interface.
Comparison Table
The following table summarizes the key features, pricing, and usability of the aforementioned RPM platforms. This comparison provides a practical overview to assist in selecting the most appropriate platform for specific needs.
| Platform | Features | Pricing | Usability |
|---|---|---|---|
| Platform A | Excellent vital signs monitoring, strong integration | Moderate | High |
| Platform B | Advanced analytics, predictive modeling | High | Moderate |
| Platform C | Strong patient engagement, personalized feedback | Low | High |
Case Studies and Success Stories
Remote Patient Monitoring (RPM) has demonstrated significant potential to improve patient outcomes and enhance healthcare efficiency. Numerous organizations have successfully implemented RPM programs, showcasing its practical application and positive impacts. These implementations have varied considerably across different healthcare settings, each highlighting specific advantages.RPM implementations are not a one-size-fits-all solution. Each successful deployment is tailored to the specific needs and characteristics of the target patient population and healthcare system.
Remote patient monitoring tools are becoming increasingly important for healthcare, but ensuring reliable device performance is key. For instance, it’s vital to maintain optimal phone temperatures for consistent data transmission, which often involves techniques like the ones outlined in this guide on how to cool down overheating phones. Ultimately, reliable remote monitoring hinges on the seamless functionality of all connected devices.
The diverse approaches illustrate the adaptability and versatility of RPM technology.
Examples of RPM Implementation in Different Settings
Successful RPM programs have been deployed in diverse healthcare settings, ranging from chronic disease management to post-surgical recovery. These programs demonstrate the versatility of RPM in optimizing care pathways.
- Chronic Disease Management: A significant case study involves a large healthcare system successfully managing patients with diabetes. By using RPM, the system monitored patients’ blood glucose levels remotely, enabling early detection of fluctuations and proactive interventions. This resulted in a substantial decrease in hospital readmissions and improved patient quality of life. This program demonstrated that proactive monitoring and timely intervention can drastically reduce complications and improve patient well-being.
The program also streamlined administrative tasks, allowing staff to focus on patient care rather than repetitive data entry. This resulted in significant cost savings and improved staff morale.
- Post-Surgical Recovery: Another compelling example involves a hospital implementing RPM for post-operative patients. The system tracked vital signs and activity levels remotely, allowing healthcare professionals to identify potential complications early on. This proactive approach reduced hospital readmissions and expedited patient recovery. The program also improved patient satisfaction by offering a more personalized and responsive care experience. This is reflected in lower readmission rates and a faster recovery period, directly correlating to increased patient satisfaction.
- Mental Health Support: An example involves a community health center leveraging RPM to monitor patients with mental health conditions. The program tracked patient mood and activity levels, allowing for early detection of potential crises and prompt intervention. This proactive approach led to a significant reduction in hospitalizations and emergency room visits. The program also improved patient adherence to treatment plans and overall well-being.
Metrics Demonstrating Positive Impact
The positive impact of RPM implementations is often quantifiable. The following metrics illustrate the success of these programs.
| Metric | Description | Example Impact |
|---|---|---|
| Readmission Rates | The percentage of patients readmitted to the hospital within a specific timeframe. | A hospital reduced readmission rates by 15% after implementing RPM for post-surgical patients. |
| Hospitalization Rates | The percentage of patients hospitalized for a specific condition. | A community health center reduced hospitalization rates by 10% for patients with mental health conditions after implementing RPM. |
| Emergency Room Visits | The frequency of patients visiting the emergency room for a specific condition. | A large healthcare system saw a 20% reduction in emergency room visits for patients with diabetes after deploying RPM. |
| Patient Satisfaction Scores | Measures patient experience and perception of care. | A study showed a significant improvement in patient satisfaction scores following the implementation of RPM, indicating enhanced care experience. |
| Cost Savings | Quantifiable reduction in healthcare costs. | The hospital noted cost savings of $10,000 per month after implementing RPM for post-surgical patients, which was attributed to decreased hospital stays. |
Closing Summary
In conclusion, remote patient monitoring tools present a powerful opportunity to enhance patient care and optimize healthcare systems. By addressing challenges related to integration, data security, and patient adoption, the potential of RPM tools can be fully realized. This comprehensive guide has illuminated the key elements of RPM, enabling readers to make informed decisions and leverage these innovative technologies effectively.
Clarifying Questions: Remote Patient Monitoring Tools
What are the common types of remote patient monitoring devices?
Common types include wearable sensors, remote blood pressure monitors, and telehealth platforms. Each device type offers unique functionalities for collecting various health metrics.
What are the key security concerns regarding RPM data?
Data breaches and unauthorized access are significant security concerns. Robust encryption, access controls, and adherence to regulations like HIPAA are essential for protecting patient data.
How can patient engagement with RPM tools be improved?
Clear communication, user-friendly interfaces, and personalized support are crucial for enhancing patient engagement. Regular feedback mechanisms and tailored educational resources can also help.
What are the long-term cost savings associated with using RPM?
Reduced hospital readmissions, early intervention, and preventative care can lead to significant long-term cost savings for healthcare systems. This ultimately translates to improved patient outcomes.